
The Obesity Epidemic and the HAES Philosophy- Can they Peacefully Coexist?

Opinion
When I first got interested in nutrition, it was because of the obesity epidemic. I was deeply disturbed by the trend in our country over the past 40-50 years of the rising number of people, who were either overweight or obese. This trend was putting more and more people at risk for developing chronic disease. Every time I’d see someone walking around who was overweight, I’d say to myself, “I wanna help shrink that person’s stomach!” But over time, I’ve learned it’s not that simple.
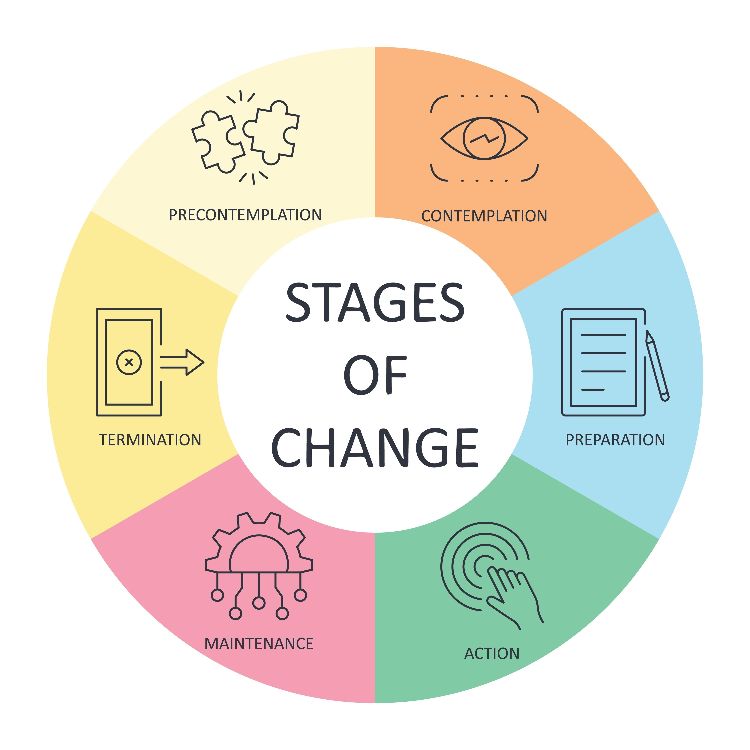
First of all, there’s something called the Transtheoretical Model. Basically, it states there’s five stages of change: precontemplation, contemplation, preparation, action, and maintenance. Most people – when it comes to weight loss – are simply not ready to take action and make that change. As well-meaning and knowledgeable that I may be on the subject of nutrition, and as much as I want to help impart that knowledge onto overweight and obese people by counseling them on modifying their diet, it’s going to fall on deaf ears if they’re not interested in changing their behavior.
I liken it to the dating world: you can’t force someone to like someone else. It’s either there or it’s not. Or by the same token, if someone is addicted to drugs, they need to be the one who realizes that rehab is the way to go. Family and friends can be well-meaning in encouraging rehab, but the drug addict ultimately needs to be the one to recognize there’s a problem, “see the light” and take corrective action. The same concept applies to an overweight or obese person- they have to be open and WANT to make that change.
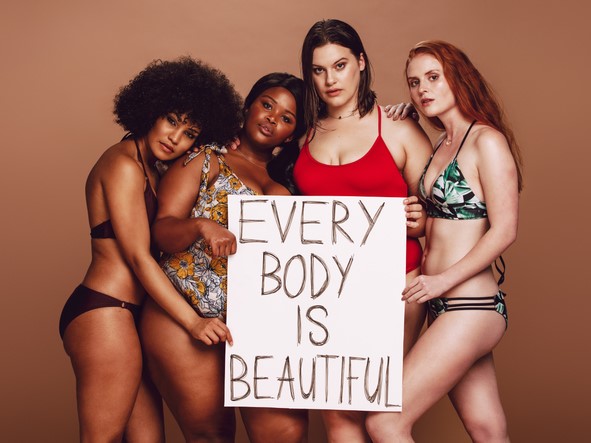
HAES Philosophy
Let me share with you an epiphany I had recently. Thanks to one of my Registered Dietitian coworkers, I now look at the obesity epidemic differently. My RD coworker introduced me to the HAES philosophy, which stands for “Healthy At Every Size.” Basically, it’s saying that we, as a society, should stop focusing on excess weight and BMI (Body Mass Index) as an indicator of health risk. Take weight out of the equation. Be body positive. Stop fat shaming. HAES proponents rightfully point out that weight loss strategies usually don’t work. And even if someone loses weight in the short-term, most people gain it back in the long-term anyhow. The focus should be more on building self-esteem and having a healthy relationship with food.
There is also some research that indicates that BMI by itself is really a poor indicator of health risk. One of the first such studies in 2013, conducted by a scientist at the CDC, concluded that being overweight (BMI: 25-29.9) – but not obese – was a protective benefit and was actually linked to a lower risk of mortality.
Furthermore, BMI has been criticized as an imperfect health indicator for another reason: Some races and ethnicities do not fall perfectly within the “normal” BMI range (18.5-24.9). For example, Asian-Americans may disproportionately find themselves in the “underweight” range, whereas Black and Latino populations may be categorized more often as “overweight” or “obese,” due to their natural body types. On the flip side, even though there are people in the “normal” BMI range, it doesn’t necessarily hold true that they are always healthy! Additionally, muscular elite athletes, who are required to do strength training to bulk up on muscle mass, end up being lumped into the “overweight” category as well, which is very misleading.
Two Things Can be True at the Same Time
To be quite honest with you, I can’t say that I embrace the HAES philosophy wholeheartedly 100%. On one hand, I agree that weight loss often doesn’t work. I concur that our society puts too much emphasis on having certain unrealistic body standards, which makes people feel self-conscious and insecure and can lead to eating disorders. I also believe that the world needs all different body types, and people should feel proud and embrace their physical appearance regardless.
On the other hand, I also am still deeply concerned about how the vast majority of Americans are either overweight or obese and how that can lead to premature deaths. It never used to be this way. I don’t want people to develop eating disorders, due to an unhealthy relationship with food, but neither do I want to see them die at an early age due to obesity which can often be modified by dietary modifications. Weight loss is hard, but the maintenance phase (6-12 months after weight loss- and possibly for the rest of one’s life) is even more challenging. I get that. But does that mean we should simply give up and stop trying?
Sources:
1.Temple NJ. The Origins of the Obesity Epidemic in the USA–Lessons for Today. Nutrients. 2022;14(20):4253. doi:https://doi.org/10.3390/nu14204253.
2. LaMorte W. The Transtheoretical Model (stages of change). Boston University School of Public Health. Published November 3, 2022. https://sphweb.bumc.bu.edu/otlt/MPH-Modules/SB/BehavioralChangeTheories/BehavioralChangeTheories6.html.
3. The health at every size® (HAES®) principles. ASDAH. April 1, 2023. https://asdah.org/health-at-every-size-haes-approach/.
4. Flegal K, Kit B, Orphana H, Graubard B. Association of All-Cause Mortality With Overweight and Obesity Using Standard Body Mass Index Categories: A systematic review and meta-analysis. JAMA. 2013 Jan 2; 309(1): 71-82.
Disclaimer: the opinions expressed in this blogpost are solely the author’s and do not necessarily reflect the opinions and beliefs of the website or its affiliates.
Art Gillman MS, RDN
Prior to becoming a Registered Dietitian Nutritionist, Art worked on public health research studies at Columbia University Irving Medical Center. Art has a MS in Nutrition Education and completed his dietetic internship in 2020, both at Columbia University’s Teachers College in NY. He has a BA in Psychology from the University of Connecticut and is bilingual in English and Spanish. Art has a passion for working with culturally diverse populations. He enjoys building rapport with community members to help them achieve optimal health.